Translate this page into:
Effect of Long-Standing Cholesteatoma in Remodelling the Temporal Bone
*Corresponding author: Rakesh Talukdar, Department of ENT, Fakhruddin Ali Ahmed Medical College, Barpeta, Assam, India. rakeshtalukdar31@gmail.com
-
Received: ,
Accepted: ,
How to cite this article: Nath RK, Talukdar R. Effect of Long-Standing Cholesteatoma in Remodelling the Temporal Bone. Ann Otol Neurotol. 2025;6:e007. doi: 10.25259/AONO_3_2024
Abstract
Chronic otitis media is the leading pathology affecting a large number of populations with various presentations. An association of cholesteatoma can aggravate the disease process, leading to complications at the time of presentation. In this paper, we present such a case of a squamosal variant of chronic otitis media with multiple complications at the time of presentation as well as during the intra-operative period. Novice surgeons should be careful, and proper guidance must be sought while operating in such a case. In addition, proper counseling must be provided to patients regarding the expected complications in the intra- as well as post-operative period.
Keywords
Cholesteatoma
Epitympanum
Facial nerve
Retro tympanum
Sigmoid sinus
INTRODUCTION
Chronic suppurative otitis media (CSOM) is often characterized by a perforated tympanic membrane (eardrum) and is associated with chronic inflammation and infection of the middle ear space (comprised of the tympanic and mastoid cavities), leading to ear discharge (otorrhea) and hearing loss. It is said to be an inflammatory process of the middle ear cleft as well as of the mucoperiosteal lining.1
Discharging ears is the most common presentation of patients attending an ENT out patient department (ENT OPD). Not all require surgical intervention, but those who do are often the advanced cases presenting with cholesteatoma residing in the middle ear cleft. The disease presides in them for decades, ending up with complications. The complications can range from facial nerve palsy to dehiscence of the semi-circular canal to various intracranial manifestations.
A cholesteatoma can be addressed as a noncancerous cystic lesion that arises from the aberrant development of keratinizing squamous epithelium in the temporal bone. It is comprised of a matrix and a central mass. It was in 1838 when German anatomist Johannes Mueller used the term cholesteatoma for the first time.2
The outcomes of ear surgery always come under the hammer as the patients are not completely satisfied. This is due to their belief in the restoration of the diseased ear from all aspects, whether it be achieving a dry ear, achieving normal hearing, etc. They fail to understand that the first and foremost aim of mastoid surgery always lies in providing a disease-free ear and to halt the extension of the disease.
Cholesteatomas are silent killers, existing in a non-aggressive state before manifesting as a potentially dangerous situation. Their capacity to release osteolytic enzymes leads to the degradation and resorption of surrounding bones and, in turn, their extension. From the eroding lenticular process of the incus to that of the semi-circular canal, the cholesteatoma can have various presentations depending on the structure involved in the complication.3
The fistula of the labyrinth is a classic complication of chronic otitis media with cholesteatoma, affecting approx. 08% of the population. It has been documented that in 90% of cases, it is the lateral semicircular canal that is affected, mainly because of its anatomical location. Other sites affected are the superior and posterior semicircular canals, oval window, vestibule, promontory, etc. A person with such a disease entity shall seldom present with otorrhea, hearing loss, dizziness, tinnitus, otalgia, headache, etc.4
The loss of overlying endochondral bone allows pressure- or mass-induced motion of underlying endosteum, perilymph, and, by contiguity, the endolymphatic compartment, thus inducing auditory and vestibular symptoms.5
The classification stated by Dornhoffer and Milewski has been widely used to grade the fistula [Figure 1].6
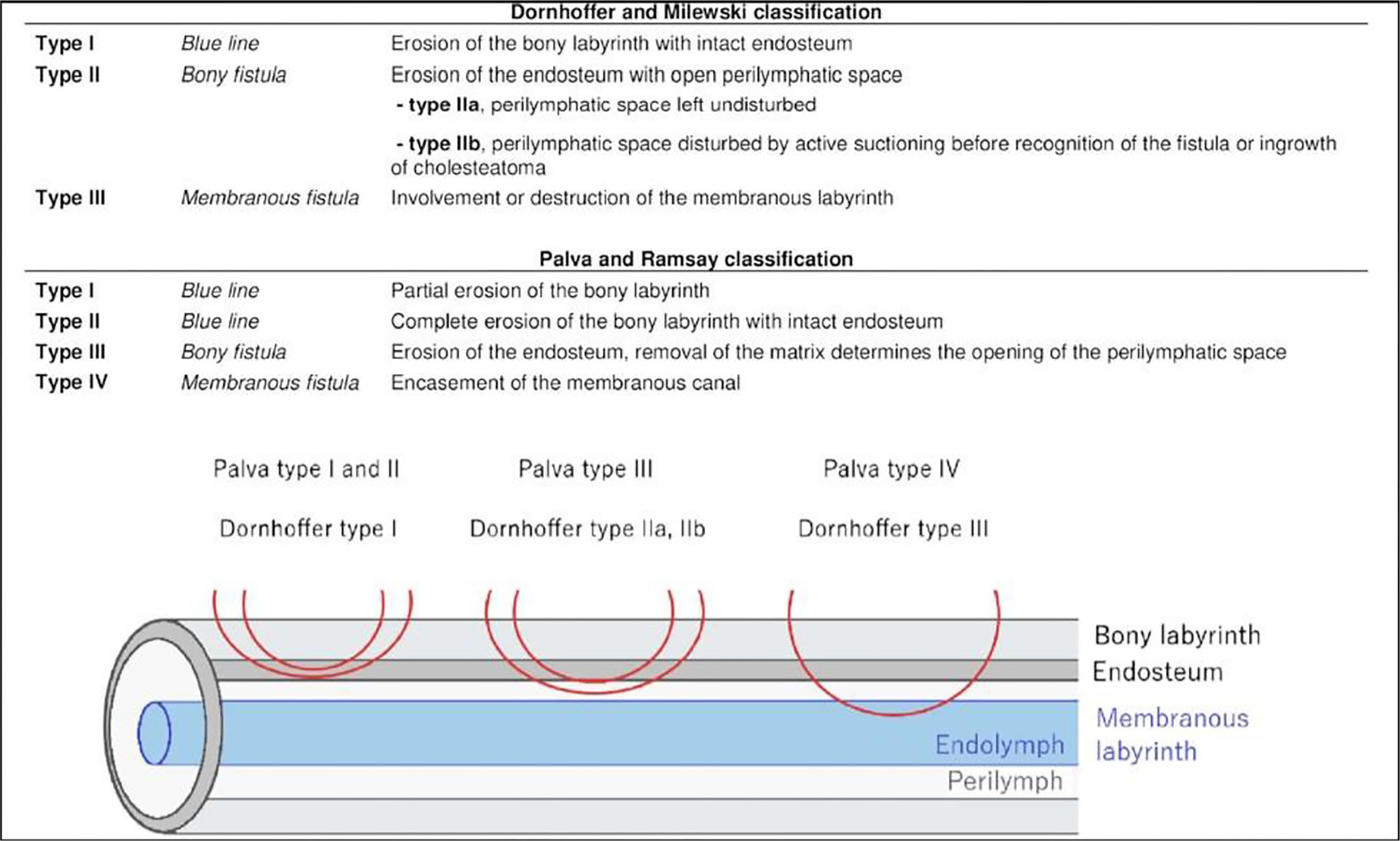

- Dornhoffer and Milewski, and Palva and Ramsay classifications of fistula extension to bony and membranous labyrinth.
Another variant, though very rare, has been associated with a case of chronic otitis media. An anteriorly placed sigmoid sinus always holds a crucial landmark. There must be no anteroposterior distance between the posterior part of the bony external auditory canal and the sigmoid sinus in order to diagnose it as a case of anteriorly located sigmoid sinus. Such cases are thought to be either a variation, being an incidental finding, or, in our case, a disease-induced osteolysis of the bone covering leading to a forward push [Figure 2].1
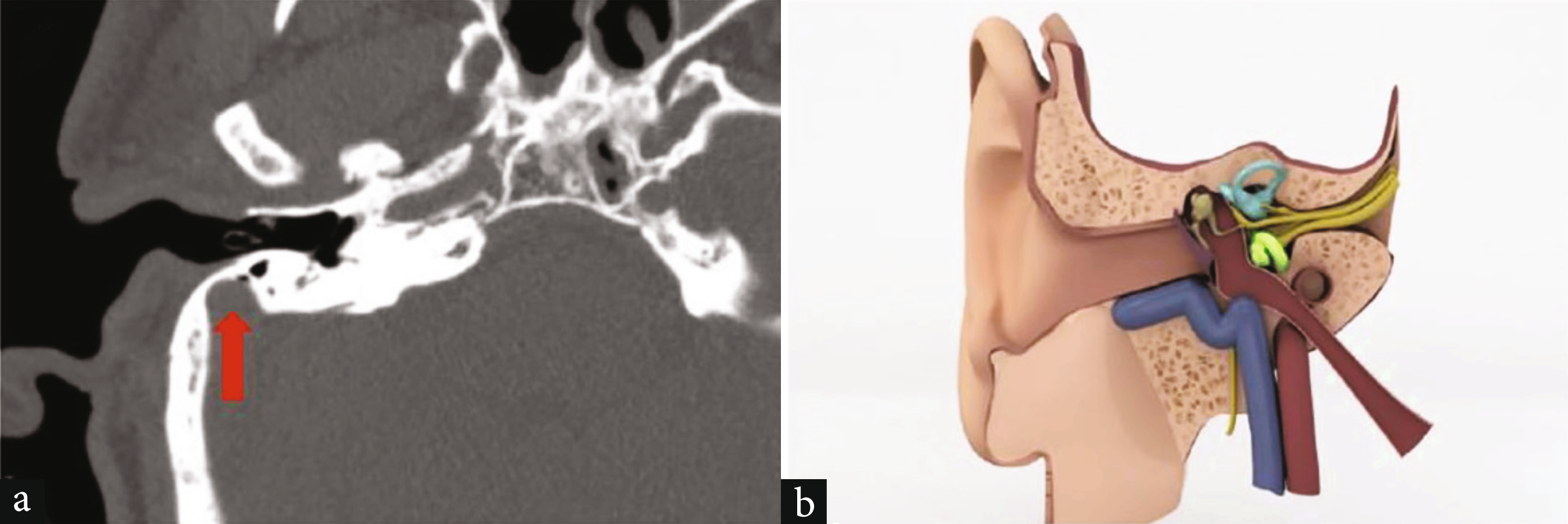
- Anteriorly located sigmoid sinus. (a) Anteriorly located sigmoid sinus. On axial CT images, it shows a sigmoid sinus very close to the outer ear (red arrow); (b) Illustration demonstrates anteriorly located sigmoid sinus. (Source- doi:10.12998/wjcc.v11.i15.3481).
Facial canal dehiscence is another entity to be kept in mind while dealing with long-standing chronic otitis media with cholesteatoma. Lots of studies have linked facial canal dehiscence and chronic otitis media, probably due to the erosive effects of enzymes [Figure 3].1
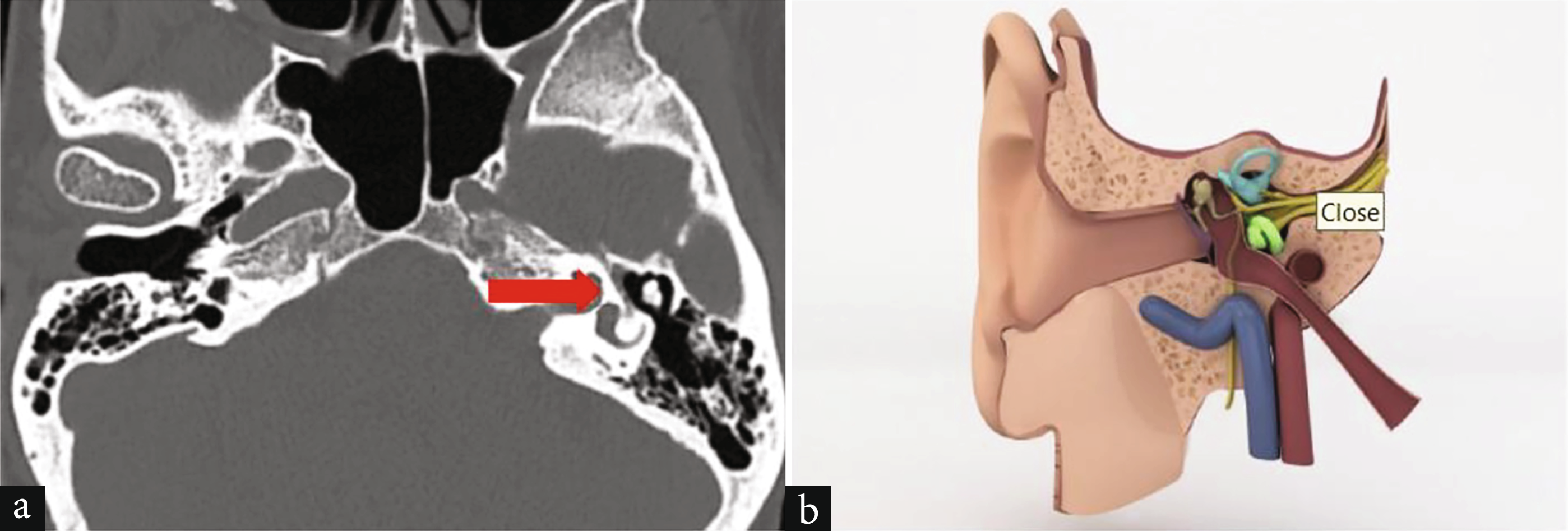
- Labyrinth segment of the facial canal without a bonny canal coverage in axial computed tomography image and illustration. (a) Axial computed tomography image shows that there is not a bonny canal coverage around the labyrinth segment of the facial nerve (red arrow); (b) In this illustration, the labyrinth segment of the facial canal can be seen without a bonny canal coverage. (Source- doi: 10.12998/wjcc.v11.i15.3481).
During middle ear or mastoid surgery, the aberrant intra-temporal course of facial nerve (FN) is the most troublesome condition. It was Fowler who first reported a series of “hump anomaly” with FN humps posterior and lateral to the prominence of the lateral semicircular canal. Surgeons are apprehensive with respect to cosmetic and functional as well as medico-legal implications associated with facial nerve injuries.7 Injury to the nerve can also result in facial disfigurement, dryness of mouth, emotional disturbances, etc.8
The most commonly affected segment is the horizontal or tympanic portion of FN. The incidence of facial canal dehiscence found during otologic surgery is usually related to chronic otitis media with cholesteatomas.9–11
Certain microdehiscence might not be reported in CT temperomastoid due to the thin structure and tortuous course of the canal. Hence, it is advised not to completely rely on CT reporting, and a descent assessment should be made of the canal intraoperatively to prevent its injury.12
In this case report, we are highlighting a rare case of chronic otitis media with cholesteatoma, a long history of 20 years, who presented us with a discharging ear, hearing loss, and CT-based reporting of lateral semicircular canal dehiscence. Yet, the patient had no history of dizziness and/or vertigo. Intraoperative findings had semi-circular canal dehiscence, exposed facial nerve, and anteriorly placed sigmoid sinus.
CASE REPORT
Case Presentation
A 65-year-old elderly lady with a known history of hypertension, dyslipidemia, and hypothyroidism attended our OPD after being referred from another tertiary care center. She had a history of chronic draining ear on the right side for a period of more than 20 years. She also had a history of gradually progressive hearing loss, and she, as well as her family members, failed to seek medical advice. There was a negative history of facial nerve palsy, dizziness, vertigo, fever with chills and rigor, or any other history or clinical features suggestive of intra-temporal and/or extra-temporal complications.
On otoscopic examination in the OPD, it was found that she had a central perforation involving both the pars tensa and pars flaccida with an exposed handle of malleus along with cholesteatoma flakes coming out of the perforation [Figure 4]. Rinne’s test was negative in the right ear, and Weber was lateralized to the affected right ear. The patient was subjected to undergo pure tone audiometry (PTA), which reported 95 dB mixed hearing loss in the affected ear [Figure 5]. To our help, she had already underwent a CT temperomastoid, which revealed soft tissue density noted in the right middle ear extending to the aditus ad antrum and mastoid air cells. The head of the malleus was found to be normal, but the handle of the malleus, incus, and stapes was eroded on the right side. It was also mentioned that there was erosion of the right lateral semicircular canal [Figure 6].
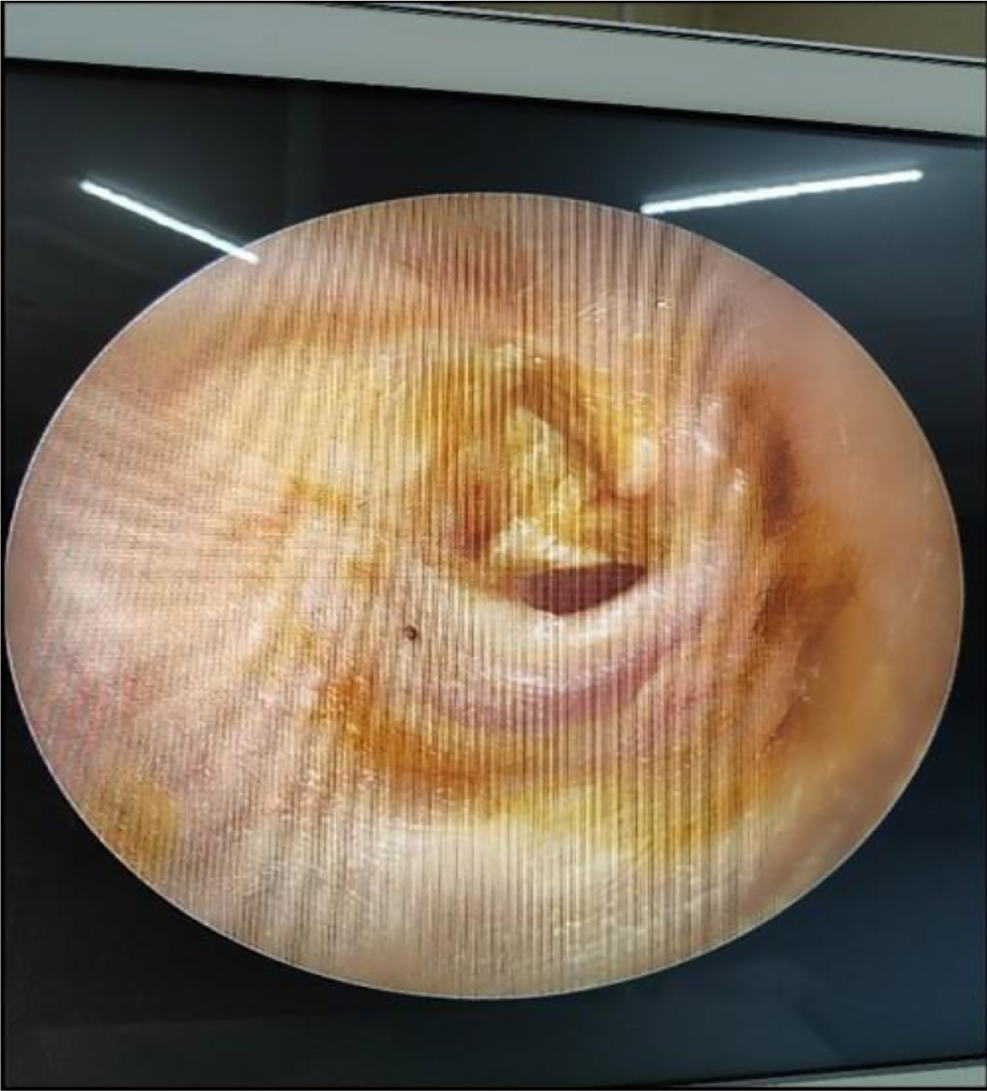
- Endoscopic view of the diseased ear.
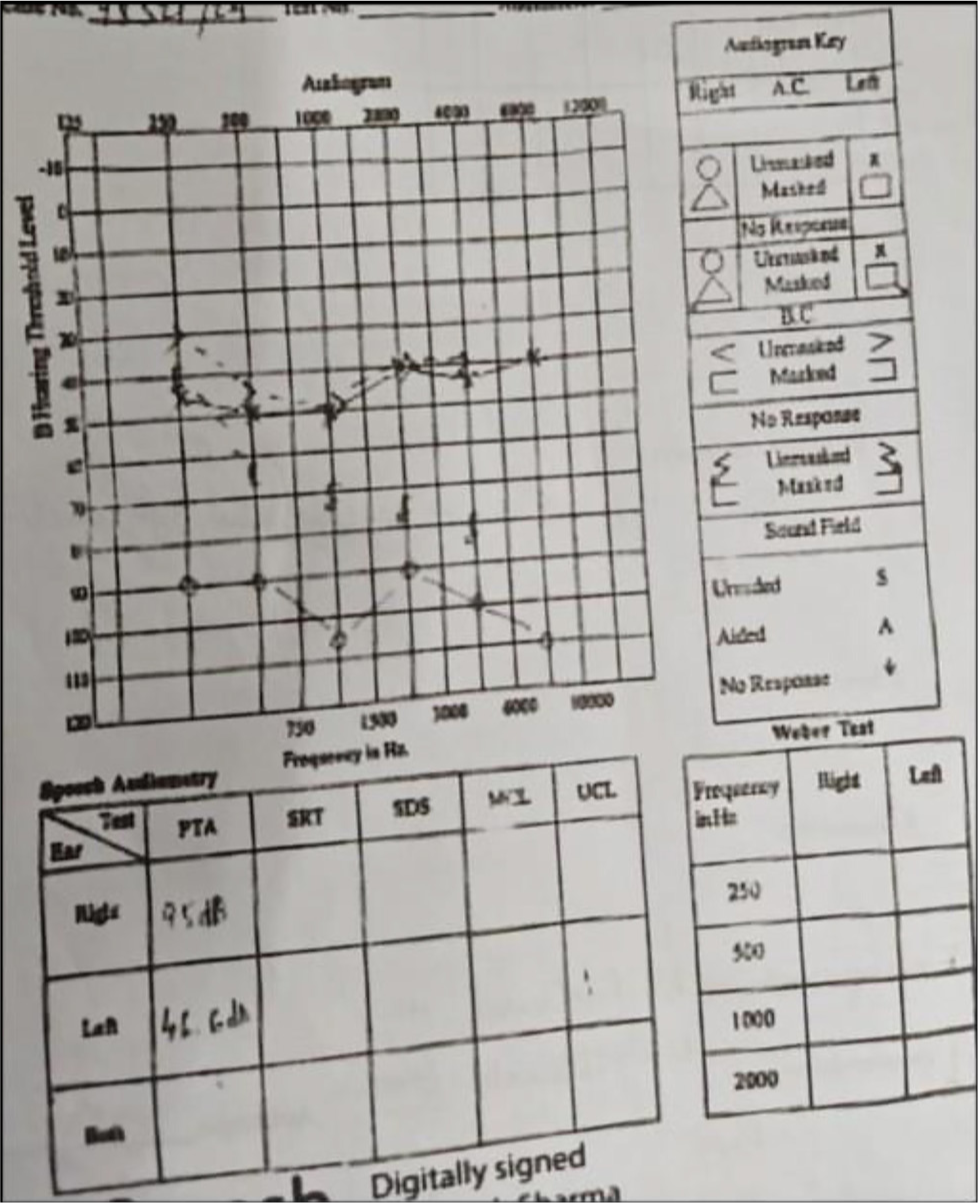
- Pure tone audiometry (PTA).
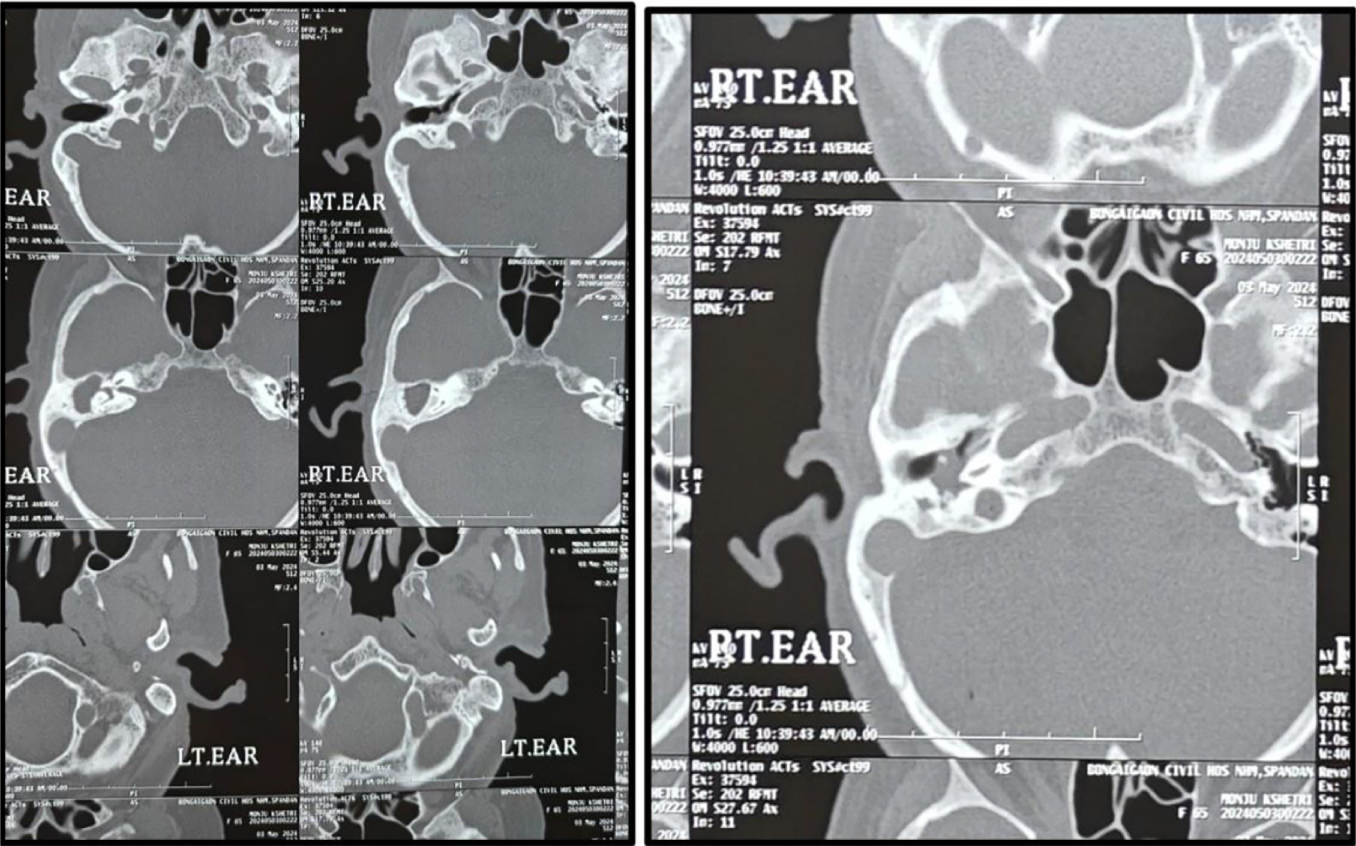
- HRCT temperomastoid showing right-sided diseased mastoid with eroded lateral SCC and an anteriorly placed right sigmoid sinus. HRCT: High resolution computed tomography, SCC: Semi circular canal.
After reading the report, Hennebert’s test was performed to check for nystagmus and was found to be absent.
After proper discussion, the patient was planned for mastoid exploration under general anesthesia (GA). Proper clearance was sought with reference to her comorbidities from respective departments as asked by the department of Anaesthesia in her pre anaesthetic check-up.
Before admitting the patient, she was started on 02% acetic acid ear drops along with antihistamines and nasal decongestants.
On the day before the surgery, the patient was made well aware of the expected complications, which included facial nerve palsy and dizziness ± vertigo pertaining to her dehiscent lateral semicircular canal.
Treatment
The patient was placed in a supine position, with the head rotated towards the left side. Upon intubation, a proper local block with 02% lignocaine with adrenaline was given in and around the pinna along with a 04 quadrant block of the EAC. Povidone-iodine (10%) was used for painting the operative region. A postauricular Wilde’s incision was made, and soft tissue dissection was done. During this step, an inferiorly based musculo-periosteal flap was harvested based on the supply of the branches of the occipital artery [Figure 7]. The spine of Henle was identified, and the posterior meatal wall was separated from the anterior mastoid wall by lifting the tympanomeatal flap. A horizontal incision was given on the posterior cartilaginous wall of the EAC and retracted forwardly. Via this route, suction clearance was done, and the margins of the perforation were made raw. A 6 mm cutting mastoid burr was used to drill the McEwan’s triangle. After a few strokes of the cutting burr, a bluish hue was encountered. Upon careful drilling around it, it was found that the sigmoid sinus was very much forward and laterally placed to such an extent that the drilling was constrained to a very small space. As the CT had already depicted a cavity being formed in the right mastoid, the mastoid antrum was easily approached. Drilling was continued till the mastoid antrum was delineated, which in this case was totally filled with cholesteatoma and its surrounding sac [Figures 8 and 9].
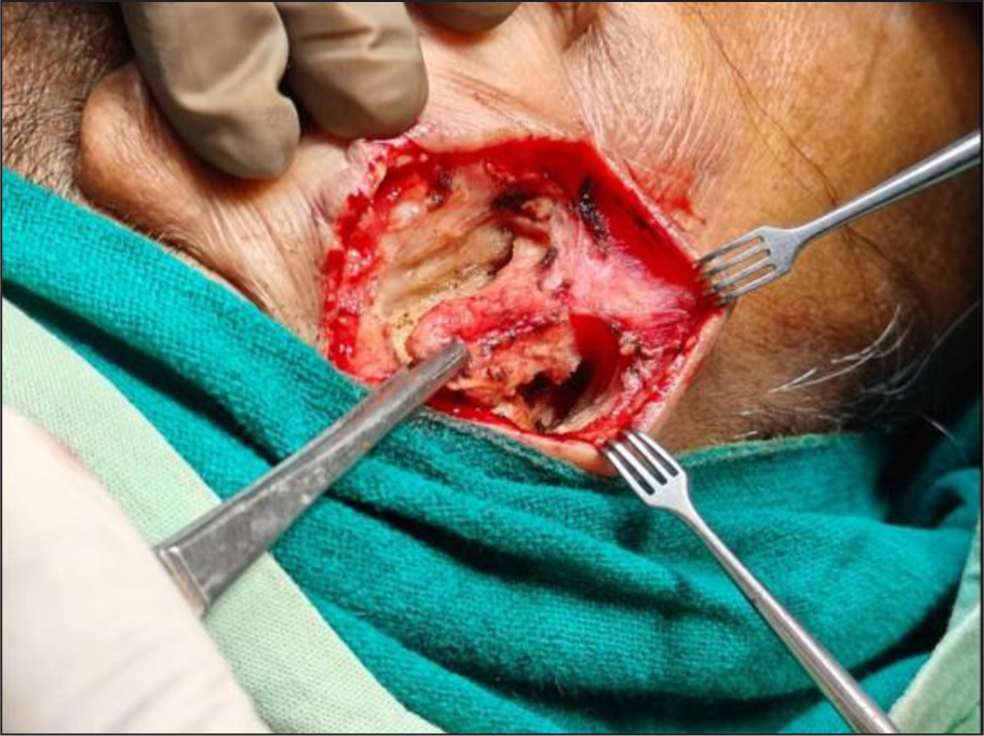
- Harvesting inferiorly based musculo-periosteal flap.
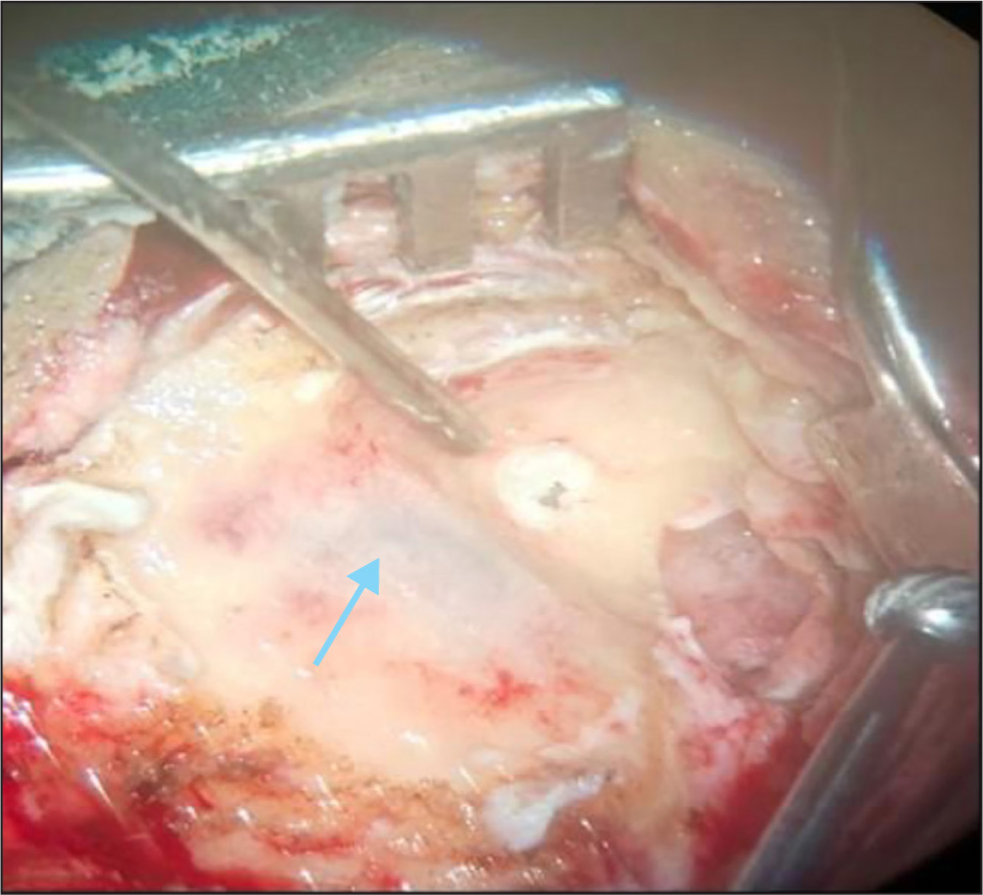
- Encountering mastoid antrum after saucerizing the sigmoid sinus (blue hue, marked with blue arrow).
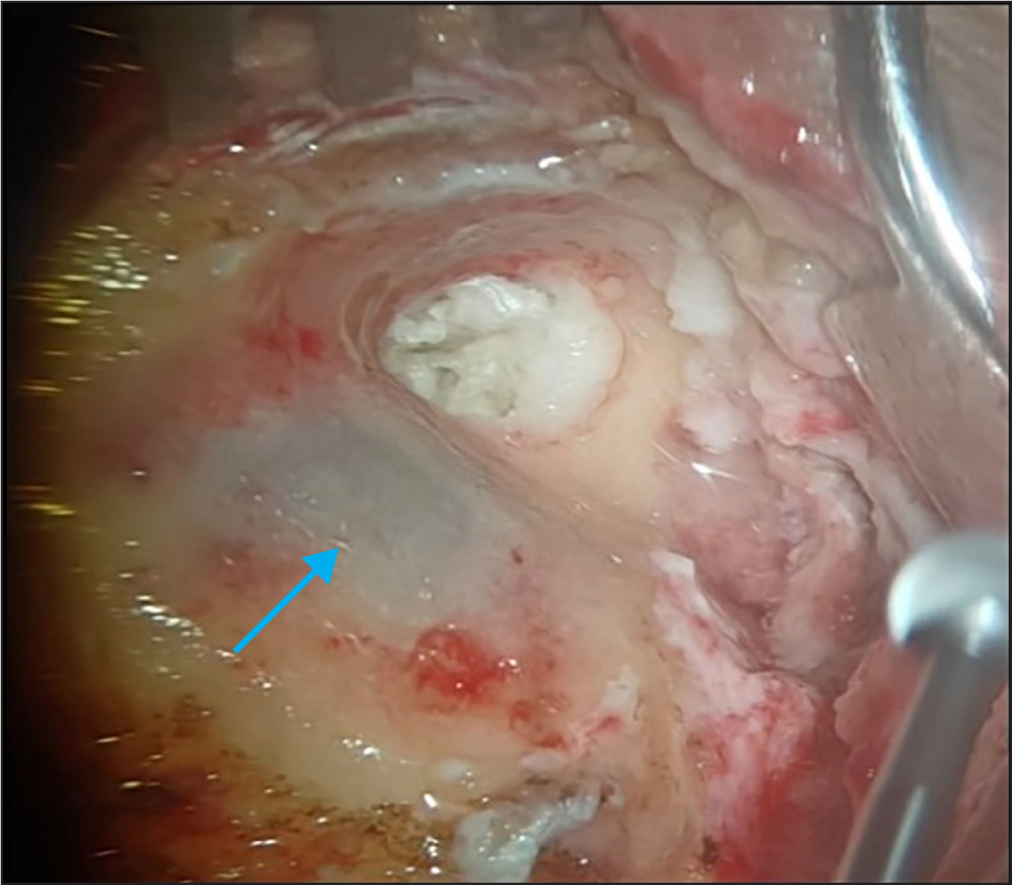
- Mastoid antrum delineated; sigmoid sinus properly seen sigmoid sinus (blue hue marked with Blue arrow).
After the antrum was drilled out, a light grayish-blue hue was noticed at the dome of lateral semi circular canal (LSCC). Upon further drilling, it was noticed that the bony LSCC was dehiscent, but the membranous portion was still intact. Just anterior to it, an exposed tympanic segment of the facial nerve was encountered. Extensive cholesteatoma extension was noticed, infiltrating the sinus tympani, facial recess, oval window niche, round window niche, epitympanum, retrotympanum, etc. The entire cholesteatoma and its sac were scooped out of the diseased places. None of the ossicles were found. Cholesteatoma had itself done an auto-mastoidectomy; hence, bringing the posterior meatal wall down was not that difficult [Figure 10].
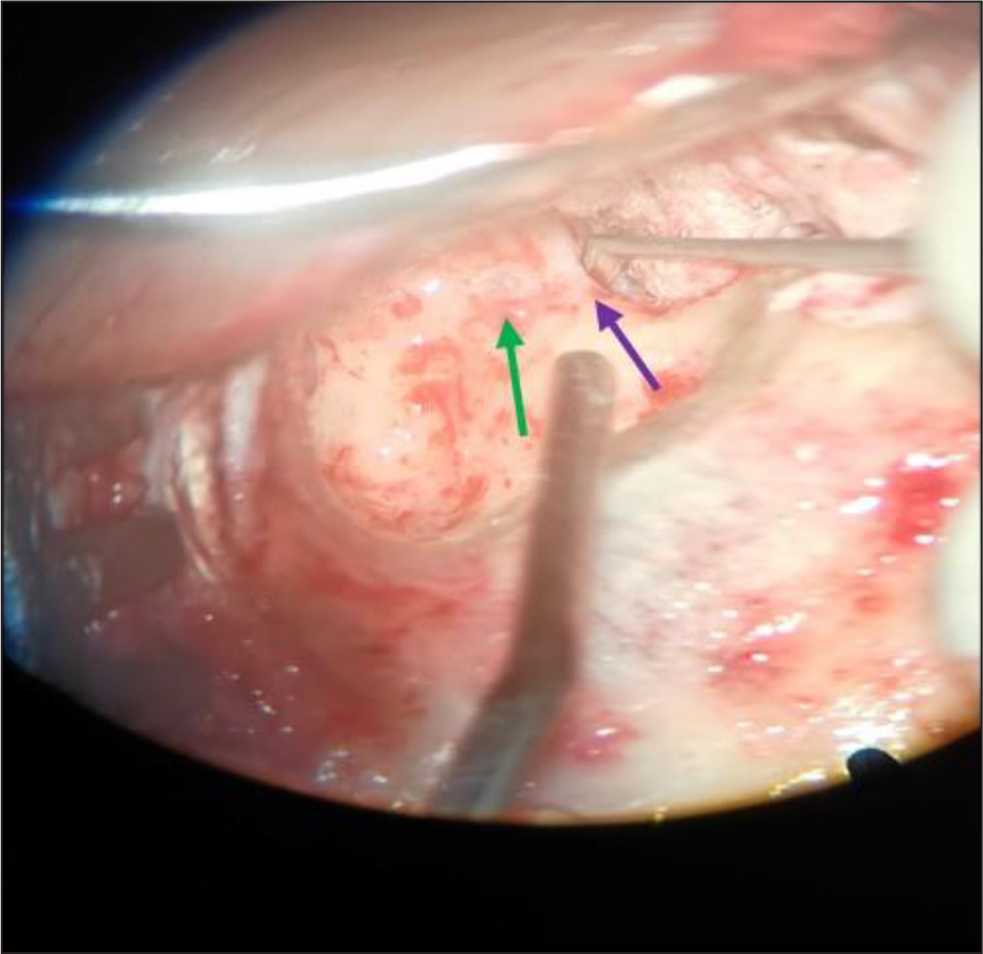
- Exposed facial nerve (purple arrow), Dehiscent lateral semi circular canal (green arrow).
Once canal wall down (CWD) mastoidectomy was achieved, temporalis fascia graft was harvested. Tympanomeatal flap was used to cover the tegmen, and the harvested graft was used to cover the dehiscent portion of LSCC. Underneath the graft, Abgel was placed [Figure 11]. Above this, the initially harvested inferior-based musculo-periosteal flap was used to obliterate the mastoid cavity. Meatoplasty was done, and an antibiotic-soaked soft roll pack was placed in situ. A postauricular dressing was done, and a compressive bandage was applied [Figure 12].
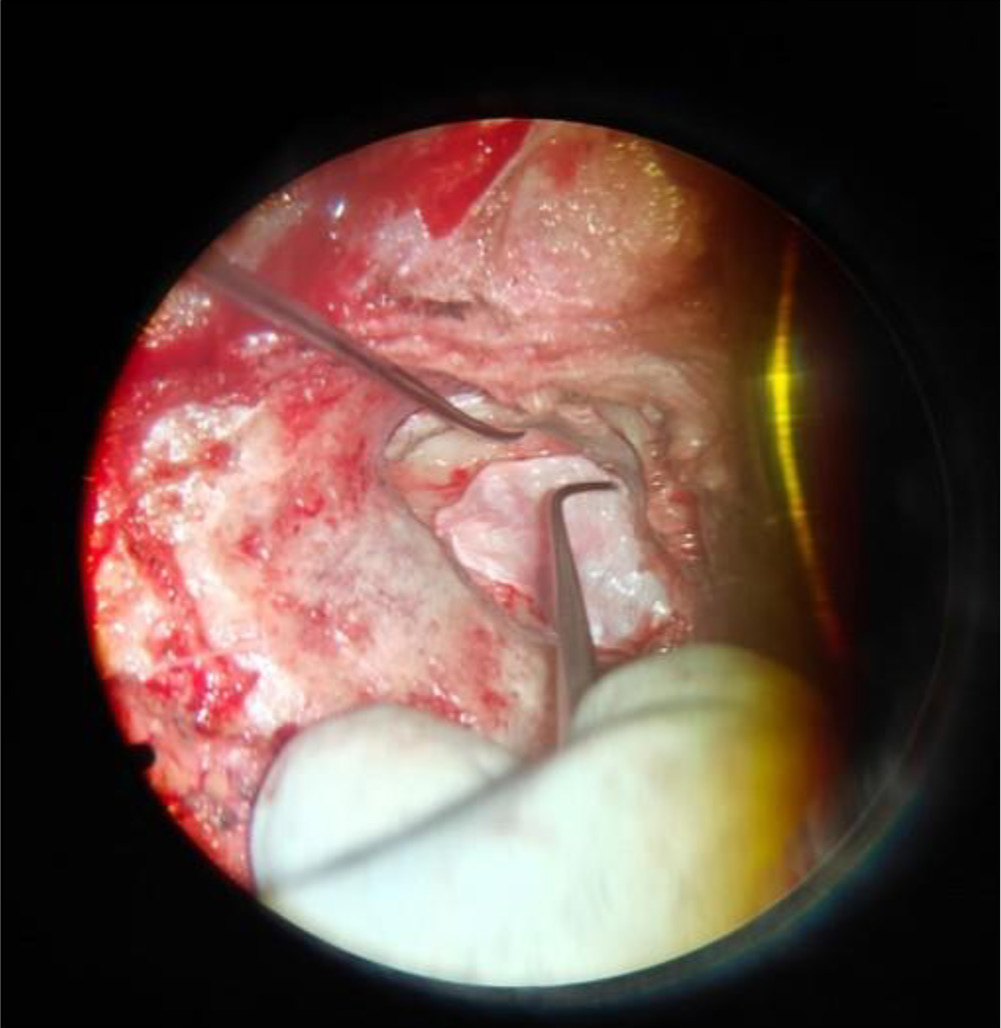
- Placing tympanomeatal flap and temporalis fascia graft. Left sided sickle knife: Tympanomeatal flap, Right sided angled probe: Temporalis fascia graft.
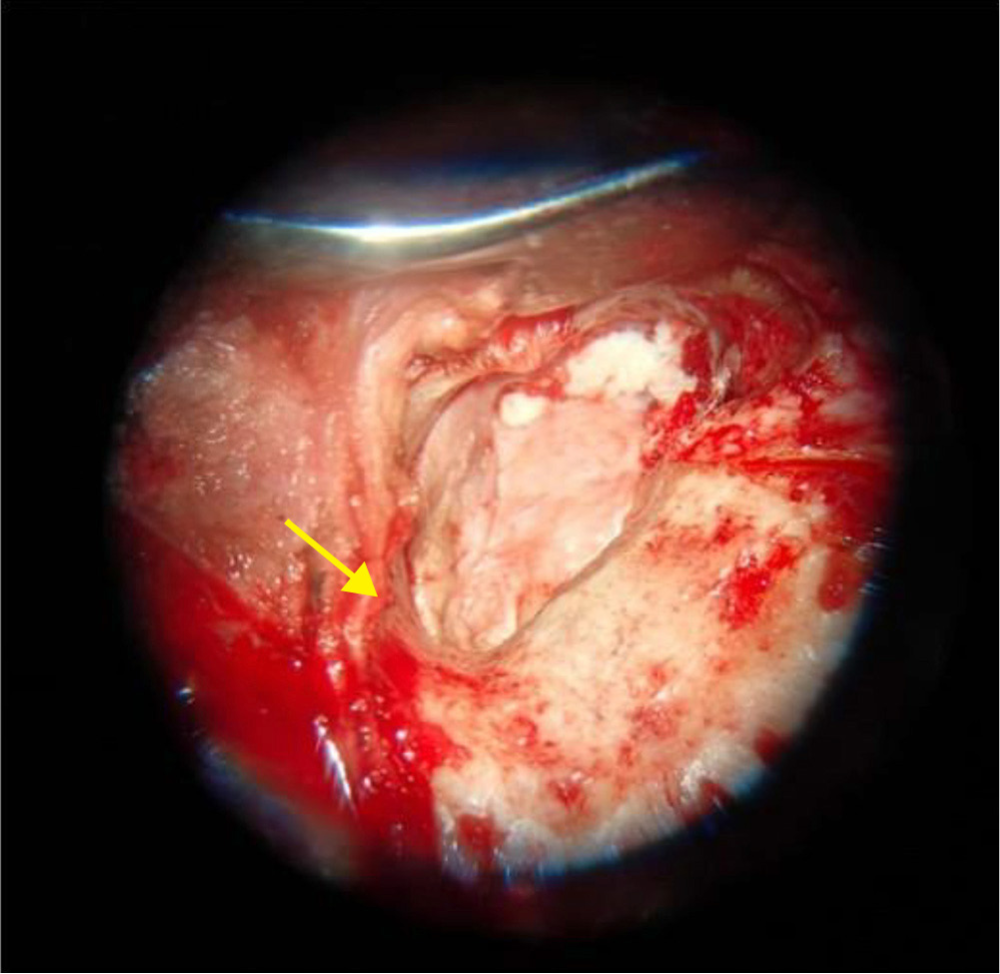
- Oblitering the mastoid cavity with inferiorly based musculo-periosteal flap, (Yellow arrow).
The patient was kept in the ward for 48 hours, during which no obvious signs of facial nerve palsy/paresis were noticed. She was discharged with oral and topical medications on the 5th day of her hospital stay.
Follow-Up
The patient came for follow-up at a 2-week interval. Postaural stitches were removed. Dried Abgel was noted in the EAC. No obvious signs of facial paralysis; signs of dizziness/vertigo were noted.
DISCUSSION
CSOM is a leading global cause of potentially preventable hearing loss in children and adults associated with low socioeconomic status. Cholesteatoma, caused by the inward growth of the squamous epithelium of the tympanic membrane into the middle ear, can also occur in long cases of chronic otitis media. In such cases, surgery to repair the tympanic membrane or remove cholesteatoma might offer long-term resolution of otorrhea and potential improvement to hearing. On the other hand, a long duration of the disease presents with it a list of complications.13
Labyrinthine fistula, one of the vestibular complications, occurs in around 8–10% of cases. Lateral semi circular canal (SCC) is the most frequent location because of its anatomical location per se. The location of a labyrinthine fistula has its own prognostic value.4
The prognosis is worse in the case of cochlear fistulas, considering that the removal of the cholesteatoma matrix over the fistula might end up inducing profound sensorineural hearing loss. Preoperative predictive signs of fistula are necessary to prevent untoward events during intra- and post-operative period.14
As per texts and data, usually elderly people with a long evolution of disease approx. Over 20 years or more of cholesteatoma otitis. Vertigo and positive fistula tests are classical signs in support of patients with bony erosion but are not always present.15
The management of such a fistula secondary to cholesteatoma remains controversial, considering two approaches are advocated. One, is leaving the matrix of cholesteatoma temporarily over the fistula, thus avoiding opening the labyrinth and, in turn, damaging the cochlear function. The other approach stated that complete removal of the matrix overlying the dehiscence should be removed, and required steps should be taken to repair the affected region. Whatever the approach followed, it is highly advised not to do suctioning over the fistula.4
The facial nerve is enclosed in the bony fallopian canal of the middle ear cavity. It has a narrow labyrinthine segment, a horizontal tympanic segment, followed by a vertical mastoid segment.
The most affected segment of the FN is the tympanic segment (8–55%). However, the abnormality associated with the vertical segment is very rare. Hohman et al.10 found that 17% of all postoperative facial nerve palsies were due to ear surgeries, 82% of which occurred during mastoid surgeries.16
FN has a very long and tortuous course within the temporal bone. Prolonged disease of the middle ear (e.g., chronic otitis media), hence, extends to the FN and affects its function. The middle ear cavity is a “Pandora box,” comprising many vital structures, the importance of which cannot be undermined nor be fulfilled accurately by other structures. The middle ear cleft bony structures and their approximation with other neurovascular structures make this region a challenging and long learning curve-based surgical site for any surgeon.8
Jugular bulbs and other venous variants have been frequently associated with tinnitus, but they should not be considered a definitive etiology of tinnitus before ruling out other possible causes because they could be often found in the general population.17
The importance of the shortest distance between the external auditory canal and the anterior edge of the sigmoid sinus (DIST) comes into play here. As per Ichijo H et al. in their study entitled “The relationship between mastoid pneumatization and the position of the sigmoid sinus,” DIST was significantly short where there was poor mastoid pneumatization. The question asked was why the DIST was significantly short where there was a poor mastoid pneumatization. Probably the chronic inflammation of the middle ear suppresses the development of pneumatization of the temporal bone.18
Even in our case, CT reporting had no comments on the sigmoid sinus, but the film showed the DIST to be significantly reduced. Intraoperatively, we did encounter an anteriorly placed sigmoid sinus.
The choice of mastoidectomy lies upon certain characteristics of the disease proper, such as its extent of bony destruction, its extension to retrotympanum, its location, etc. But, the choice of surgical procedure itself does not hold security for attaining disease-free and non-complicated post-op status. The experience of the surgeon in identifying the abnormalities in the pre-op status as well as in the intraoperative stage holds true for minimizing complications.6
Bezold once wrote, “an incompetent operator, who is not aware of many anatomical details crowded together in the narrow space of the temporal bone and their extreme variability, poses a much greater danger to the patient than in any other regions of the body.”19
The overconfidence of experienced surgeons and the under-preparedness of the novice who do not expect to see any unusual findings in the course of the disease have been considered to be the leading causes of iatrogenic injuries to this structure.8
CONCLUSION
The idea behind preparing this case was to put forward the effect of the long-standing state of chronic otitis media on the temporal bone. In this single case, we highlighted three abnormalities, namely, dehiscent lateral semicircular canal, exposed facial nerve, and anteriorly placed sigmoid sinus. Being a diseased mastoid for over 20 years, providing a disease-free state in the post-op state held great difficulties in the operative stage.
Otorhinolaryngology per se is a pleomorphic subject; otological surgeries, on the other hand, are very challenging with respect to the hand-eye coordination needed to accomplish the surgery. Hence, fruitful outputs can only be achieved if the novice has enough visualization of the anatomy and the variations associated with it, taking utmost precaution to identify any such anomalies in the pre-op as well as intra-op status.
Ethical approval
Institutional Review Board approval is not required.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
Use of artificial intelligence (AI)-assisted technology for manuscript preparation
The authors confirm that there was no use of artificial intelligence (AI)-assisted technology for assisting in the writing or editing of the manuscript and no images were manipulated using AI.
REFERENCES
- Chronic Otitis Media and Middle Ear Variants: Is There Relation? World J Clin Cases. 2023;11:3481-90.
- [CrossRef] [PubMed] [PubMed Central] [Google Scholar]
- Diagnosis and Treatment Modalities of Cholesteatomas: A Review. Cureus. 2022;14
- [CrossRef] [PubMed] [PubMed Central] [Google Scholar]
- Management of Advanced Cholesteatoma: Madras ENT Research Foundation Experience. Int J Otorhinolaryngo Head Neck Surg. 2020;6:1149.
- [Google Scholar]
- Lateral Semicircular Canal Fistula in Cholesteatoma: Diagnosis and management. Eur Arch Oto-Rhino-Laryngol. 2016;273:2055-63.
- [CrossRef] [PubMed] [Google Scholar]
- Cholesteatoma Labyrinthine Fistula: Prevalence and Impact. Braz J Otorhinolaryngol. 2019;85:222-7.
- [CrossRef] [PubMed] [PubMed Central] [Google Scholar]
- Presentation, Management, and Hearing Outcomes of Labyrinthine Fistula Secondary to Cholesteatoma: A Systematic Review and Meta-Analysis. Otol Neurotol. 2022;43:E1058-68.
- [CrossRef] [PubMed] [Google Scholar]
- Facial Nerve Lying Lateral to Ossicles in One Case of Congenital Aural Atresia. Int J Pediatr Otorhinolaryngol. 2011;75:597-9.
- [Google Scholar]
- Classification of Facial Nerve Aberration in Congenital Malformation of Middle Ear: Implications for Surgery of Hearing Restoration. J Otol. 2018;13:122-7.
- [CrossRef] [PubMed] [PubMed Central] [Google Scholar]
- Aberrant Course of Facial Nerve in the Middle Ear Cavity. Indian J Otol. 2020;26:197-8.
- [Google Scholar]
- A Rare Case of Aberrant Facial Nerve Course in the Mastoid Segment. Polski Przegląd Otorynolaryngol. 2021;10:30-3.
- [Google Scholar]
- Anatomical Features of Intratemporal Course of Facial Nerve and Its Variations. Cureus. 2018;10:e3085.
- [CrossRef] [PubMed] [PubMed Central] [Google Scholar]
- Micro-CT Study of the Dehiscences of the Tympanic Segment of the Facial Canal. Surg Radiol Anat. 2017;39:375-82.
- [CrossRef] [PubMed] [PubMed Central] [Google Scholar]
- Treatment of Labyrinthine Fistula. Available from: http://archotol.jamanetwork.com/. [Last accessed date 03 July 2024]
- [Google Scholar]
- Cholesteatoma Surgery: Management of the Labyrinthine Fistula—A Report of 97 Cases. Laryngoscope. 1979;89:78-87.
- [CrossRef] [PubMed] [Google Scholar]
- Our Experience of Anatomical Variations of Facial Nerve in Cadaveric Temporal Bone Dissection. Indian J Otolaryngol Head Neck Surg. 2021;73:271-5.
- [CrossRef] [PubMed] [PubMed Central] [Google Scholar]
- The Ear, the Surgeon and the Radiologist. Hickey Lecture, 1973. Am J Roentgenol Radium Ther Nucl Med. 1973;118:501-10.
- [CrossRef] [PubMed] [Google Scholar]
- The Relationship Between Mastoid Pneumatization and the Position of the Sigmoid Sinus. Eur Arch Otorhinolaryngol. 1996;253:421-4.
- [CrossRef] [PubMed] [Google Scholar]
- Imaging the Facial Nerve: A Contemporary Review. Radiol Res Pract. 2013;2013:1-14.
- [CrossRef] [PubMed] [PubMed Central] [Google Scholar]








